One year ago, healthy 14-year-old Amelie suddenly began having severe stomach pain, nausea and abdominal cramping. Initially, Amelie assumed she had a bad case of the stomach flu, but her symptoms continued for four months.
Amelie experienced rapid weight loss and anxiety around eating, prompting her parents to seek out help from the experts at CHOC. After initial consultations, Amelie had a team of CHOC gastroenterologists, psychologists and dietitians working together to diagnose and treat her illnesses. CHOC’s multidisciplinary approach and expert collaboration allowed Amelie to get back to eating her favorite foods — pain and anxiety free.
Severe stomach pain
When Amelie’s flu-like symptoms persisted for weeks, her mom Angelika took her to their primary care physician to be assessed. They were about to leave on a trip to Europe for a month and were nervous about the condition of Amelie’s health.
Their doctor assured Angelika and Amelie that her stomach pain was due to anxiety and encouraged them to enjoy their trip. But while abroad, Amelie’s condition worsened. She stayed in bed for most of the trip with extreme stomach pain and just not feeling like herself. Then, she began to not be able to go to the bathroom at all.
Meanwhile, Angelika was frantically searching pharmacies for advice and medicine. They tried various medications to help, but Amelie began rejecting all food, water and medicine in fear that they would make her stomach hurt. When Angelika finally convinced Amelie to eat a piece of toast, she couldn’t even get it down.
“I took one bite and I immediately started freaking out,” says Amelie. “It was stressful because we didn’t have any medication and we didn’t know what was going on.”
Seeking answers at CHOC
Amelie’s family returned to America determined to get some answers, especially because Amelie was due to start high school in two weeks. They revisited their primary care physician and were referred to CHOC. At CHOC, Amelie received a series of tests: ultrasounds, bloodwork, an endoscopy and a colonoscopy. All the tests came back normal.
“Every time a test came back clean, it felt like being punched in the face,” says Amelie, “There was nothing visibly wrong, but I clearly wasn’t doing OK. The pain was unbearable.”
Amelie’s diet consisted of ground turkey, white rice and rye bread. She would only eat once or twice a day and her weight was dropping rapidly. She was so malnourished that she began having trouble walking and was experiencing fainting episodes.
On her first day of high school, Amelie left early and never returned; she switched to homeschooling due to her ongoing pain and fatigue.
“Homeschooling was a good option for me, but it was hard to explain what was happening when friends asked me. I would just say, ‘Oh I have stomach pain,’” says Amelie. “I gave everyone a short snippet of what was happening. I was crying all the time and literally pulling my hair out because I was so stressed.”
Because of her low-calorie intake and hesitation to eat, many thought that Amelie had anorexia. However, Amelie and Angelika could not make any sense of that since she was not trying to lose weight and nor did she feel that she needs to lose any.
Dr. Gregory Wong, a pediatric gastroenterologist at CHOC, was the first to recognize that Amelie’s issues with eating are not from an eating disorder like anorexia but from the fear of eating created by her gastrointestinal (GI) symptoms. Dr. Wong worked with Amelie to develop a plan to reduce her anxiety and disordered eating. He then referred her to be seen in the Functional Abdominal Pain Program at CHOC.
Small intestinal bacterial overgrowth (SIBO)
When Amelie and Angelika met with Dr. Ashish Chogle, pediatric gastroenterologist and director of the Functional Abdominal Pain Program, they described him as “a breath of fresh air.” He was able to figure out and explain what was causing Amelie’s GI issues within 10 minutes of talking to her.
Turns out, Amelie’s abdominal pain most likely started with a stomach bug. Then, the stomach bug may have triggered nerve malfunction in her gut. These nerves led the gut to become hypersensitive and lead to pain while eating. The malfunctioning nerves also affected gut movement, leading to constipation and unwanted bacterial overgrowth called small intestinal bacterial overgrowth (SIBO).

SIBO causes an imbalance of the microorganisms in the gut that maintain healthy digestion. When too many bacteria, of the wrong kind, populate the small intestine, it can cause pain, nausea, diarrhea, constipation, gassiness and bloating — much like it did for Amelie.
Neuro-stimulation through IB-stim device
To treat Amelie’s SIBO, Dr. Chogle prescribed antibiotics to kill the bad bacteria and then asked Amelie to take probiotics to have the good bacteria replace the bad ones in her intestines.
To address the nerve malfunction, he recommended neuro-stimulation through IB-Stim, a small device that would be placed behind Amelie’s ear. The IB-Stim device sends subtle electrical pulses through short wires and tiny needles taped to the ear. These gentle stimulations improve the functioning of the nerves that control the pain sensation and motility of the gut.
With the IB-Stim treatment, the patient will typically wear a device for five days, have two days off and then a new device would be placed once a week for four consecutive weeks.
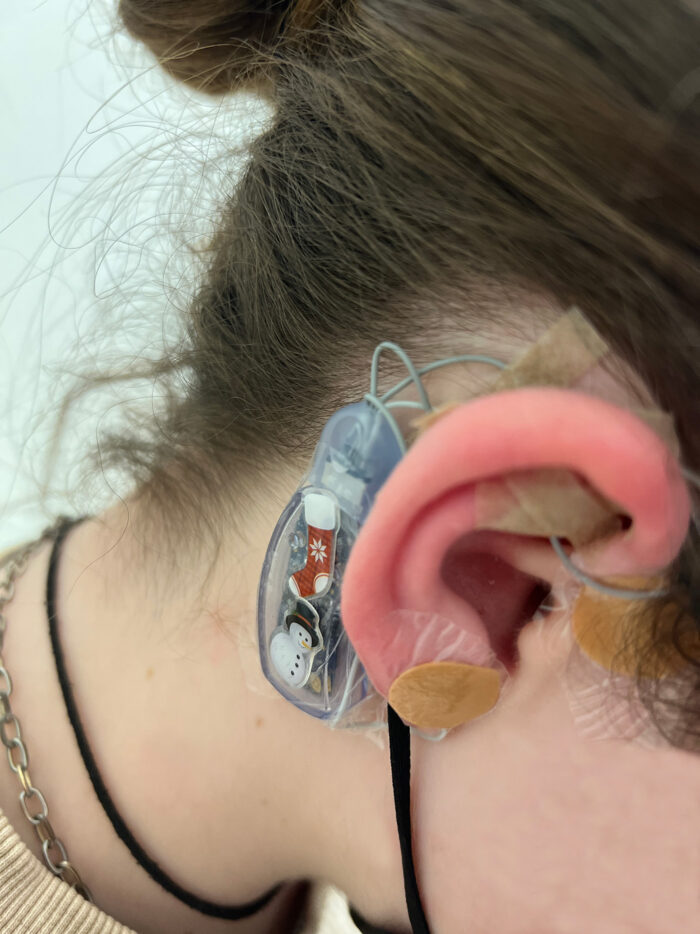
Tammy Tran, nurse practitioner at the Functional Abdominal Pain Program, would place the device once a week and check on Amelie’s symptoms. Amelie loved Tammy’s positive spirit and constant encouragement during these treatments. Tammy has placed over 2,000 IB-Stim devices since the clinic began under Dr. Chogle’s leadership.
“I did two rounds of IB-stim,” says Amelie. “It’s crazy how it works.”
Amelie’s nerves were back in rhythm, her gut bacterial health was reestablished and her stomach pain was gone.
This was great news, but another problem remained; Amelie was still afraid to eat.
Avoidant restrictive food intake disorder (ARFID) and anxiety
Rather than anorexia, Amelie had actually developed avoidant restrictive food intake disorder (ARFID). ARFID is an eating disorder in which different foods are avoided unrelated to distress about body shape or size. Developing ARFID is common with gastrointestinal disorders. About 25% of the children with disturbances in their gut and brain nerve functioning typically develop some form of ARFID.
Amelia often worried about her stomach pain and if the food would make it worse. Then, focusing on that worry caused her to be anxious— often pacing, pulling her hair out and scratching herself. She had developed what is called anticipatory anxiety about eating.
The Functional Abdominal Pain Program at CHOC works with pediatric gastroenterologists, nurse practitioners, dietitians, psychologists, care coordinators, and nurses to develop a treatment plan that can help families manage both the physical and psychological impacts that abdominal pain can cause.
With help from medication, gut-directed hypnotherapy and breathing skills, Amelie’s anxiety began to subside.
Read CHOC’s ultimate guide to helping kids and teens overcome eating disorders.
Strawberries by summertime
Getting back to having a diverse diet took a bit longer though, and Amelie was losing hope. She started to work closely with GI dietician Katherine Bennett. Katherine worked with Amelie to slowly introduce new foods back into her diet in a non-stressful, pain-free way.
Amelie told Katherine — whom she calls her biggest cheerleader — that it was her goal to be able to enjoy strawberries by summertime.

She achieved that goal; now, she says she eats two cartons a day.
This summer, Amelie was able to return to Europe with her family and eat all the different foods she had missed out on during her last visit.
“I’m making up for lost time,” says Amelie.
Amelie still comes to CHOC to see Dr. Chogle for routine appointments, but she can eat whatever she wants and enjoy life pain-free — all because of the compassionate and expert care she received at CHOC.
Get more expert health advice delivered to your inbox monthly by subscribing to the KidsHealth newsletter here.
Learn more about the gastroenterology (GI) program at CHOC
Our gastroenterology team is committed to offering patients the very latest treatments in an environment dedicated to patient- and family-centered care.





