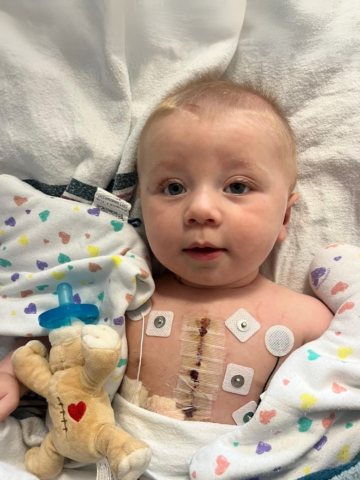
Olivia was unexpectedly born two months premature and spent the first seven months of her life in the CHOC neonatal intensive care unit (NICU). During some moments of their extended NICU stay, her parents weren’t sure if they would ever get to take their baby girl home.
From the day she was born, Olivia had been exposed to a high level of stimulation in the hospital setting. Despite the NICU’s environment of healing, the beeping of machines, and steady flow of clinicians in and out of her room had overwhelmed Olivia and made her weary of physical touch.
“Even though the doctors and nurses were very gentle with her, and everything was done with her best interest in mind, it’s a natural outcome for someone who has spent their entire life thus far in a hospital to be apprehensive of physical touch,” says Leilani, Olivia’s mother.
The NICU’s developmental team quickly saw that Olivia would benefit from music therapy, and introduced Olivia’s family to Brie Mattioli, a board-certified music therapist at CHOC who specializes in the NICU setting.
Initial goals of music therapy for Olivia included pain management, learning how to self-soothe, and self-regulation. Once her pain improved, she could show more self-expression and even develop preferences for certain types of music. (Her favorite song is “Rise Up” by Andra Day.)
Sometimes Brie’s goal was to help Olivia get to sleep, which is healing. During other sessions, their goals were focused on development and stimulation.
The calming effects of music therapy was just what Olivia needed.
Afterall, she underwent her first in a series of surgeries when she was just 2 weeks old. During prenatal scans, doctors discovered that Olivia had enlarged kidneys, and at birth they discovered her stomach was enlarged as well. Surgery was a priority. Under the care of Dr. Peter Yu, pediatric general and thoracic surgeon, Olivia’s intestines were repaired. Another surgery, when Olivia was 2 months old, shortened her lengthy spinal cord.
Olivia also showed traits of Noonan Syndrome ― a rare genetic disorder that affects one in 1,000 to one in 2,500 people. Noonan Syndrome is commonly associated with physical characteristics like atypical facial characteristics and a short stature, and clinical symptoms like heart defects, bleeding problems, feeding issues, developmental delays and malformations of bones in the rib cage. Although Olivia seemed to exhibit mild physical characteristics of the syndrome, she displayed prominent clinical symptoms.
While she underwent genetic testing for Noonan Syndrome, Olivia’s care team also indicated that she was a candidate for genomic sequencing, the process for determining someone’s complete DNA sequence. Through a partnership with Rady Children’s Hospital, some critically ill infants and children in CHOC’s intensive care units have access to rapid whole genome sequencing. The research collaborative intends to decrease the time between an acute diagnosis and the implementation of effective treatment for difficult-to-diagnose cases. Olivia was genetically tested as were her parents. Two weeks later, the results came in. Neither parent tested positive for Noonan Syndrome, but Olivia did. Since neither parent was a carrier, this meant that Olivia had a uniquely altered gene that resulted in the syndrome.
“When the results came back, we were in disbelief and grieving,” Leilani recalls. “The news was unexpected and heartbreaking. We had never heard of Noonan Syndrome and we had done most of the genetic testing offered during my pregnancy. Our baby was so innocent, and she didn’t ask for any of this. I found myself fast-forwarding to the future and wondered what life would look like for her.”
Music as a journey to healing
While in the hospital, Olivia saw Brie four times a week for music therapy. The more music therapy sessions Olivia had, the more relaxed she became in a sometimes-stressful hospital environment.
“When bodies are relaxed, they heal better,” Brie says. “More opportunities for relaxation mean more opportunities for healing, positive gains and progress.”
In addition to helping patients make progress towards clinical goals, music therapy can provide a sense of normalcy to families in the midst of an emotional time.
“Music promotes a sense of positivity and peace in the room,” Brie says. “It wasn’t the nursery they planned to bring their baby home to, but it provides a sense of normalcy to families.”
The practice resonated with Leilani, who had even considered pursuing a career in music therapy in college. While pregnant with Olivia, she would frequently play music, everything from Ed Sheeran to N*SYNC for her daughter.
“My pregnancy was difficult, and music had always been a form of therapy to me,” Leilani says.
When Olivia was discharged from the NICU, her parents were given a CD specially recorded by Brie with Olivia’s favorite music therapy songs so she could continue healing at home.
“No parent signs up to be in the hospital for all those months,” Leilani recalls. “But I am so happy that CHOC was there when we needed them. CHOC was the right place for Olivia.”
Get more expert health advice delivered to your inbox monthly by subscribing to the KidsHealth newsletter here.

Learn more about CHOC’s Neonatology Services
CHOC Hospital was named one of the nation’s best children’s hospitals by U.S. News & World Report in its 2025-26 Best Children’s Hospitals rankings and ranked in the neonatology specialty.